(951) 779-8862
Why a Personalized Hygiene Plan Is the Real Key to Implant Success

By Inland Choice Dental | March 10, 2026
Most people do their research before getting implants — the procedure itself, the recovery timeline, and the cost. What rarely gets enough attention is what happens after the implant is placed. Specifically, how you care for it every single day. That’s where a personalized hygiene plan comes in, and it makes a much bigger difference than most patients expect.
What Makes Implant Care Different From Regular Dental Hygiene
Implants look and function like natural teeth, but they aren’t identical to natural teeth under the gum line. Natural teeth have a periodontal ligament — a fibrous tissue that connects the tooth root to the jawbone and helps buffer force. Implants fuse directly to the bone through a process called osseointegration. That means the surrounding tissue has less natural defense against bacterial invasion.
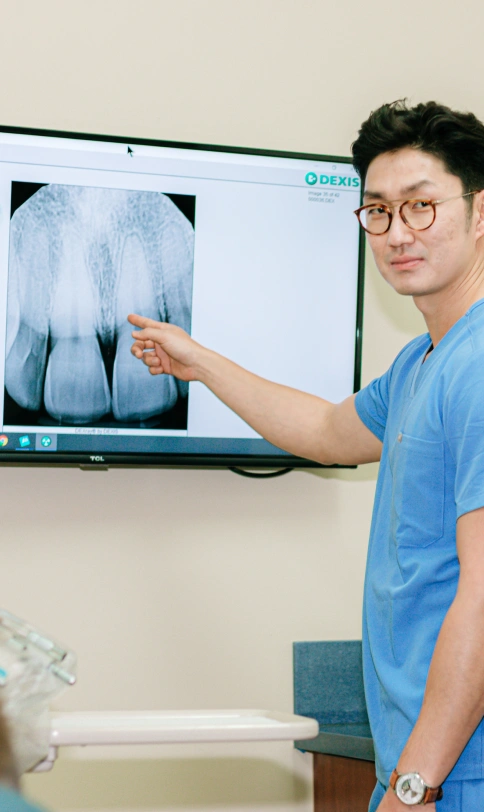
For patients who’ve received dental implants in Riverside, this distinction matters from day one. Without the right cleaning habits, bacteria can accumulate around the implant base, leading to peri-implantitis, a condition similar to gum disease that can cause bone loss and implant failure. Research published in the Journal of Clinical Periodontology found that peri-implantitis affects an estimated 22% of implant patients. That number doesn’t have to include you.
Why One-Size-Fits-All Instructions Fall Short
Generic post-procedure instructions — “brush twice a day, floss regularly” — aren’t enough on their own. The condition of your mouth matters: the position of the implant, the health of your gum tissue, whether you have a bridge or a single crown, your bite pattern, and your history with gum disease. All of it shapes what your daily routine needs to look like.
A personalized hygiene plan accounts for these variables. It’s not about adding complexity to your routine; it’s about making your routine actually work for your mouth’s anatomy and conditions.
What a Personalized Plan Includes
A well-designed hygiene plan for implant patients typically covers several specific areas:
- Brushing technique: Soft-bristled brushes with a 45-degree angle matter more around implant crowns. Electric toothbrushes with pressure sensors help avoid aggressive brushing that can irritate the tissue around the implant.
- Interdental cleaning: Floss threaders, water flossers, or interdental brushes are often recommended depending on the spacing around your implant. Regular floss alone sometimes misses the zone directly beneath the crown.
- Low-abrasive toothpaste: Some whitening toothpastes contain abrasive particles that can scratch the implant surface over time, making it more prone to bacterial adhesion.
- Antimicrobial rinse: For certain patients — especially those with a history of gum disease — a prescribed rinse can significantly reduce bacterial load around the implant.
- Diet and habit guidance: Smoking, excessive alcohol, and a diet heavy in refined sugars all compromise gum tissue health and slow osseointegration. Your hygiene plan should address these if they apply.
None of these points is radical. But knowing which apply to you, and in what combination, is what separates a plan that works from one that’s just going through the motions.
The Role of Professional Cleanings in Long-Term Implant Health
Home oral care is only part of the equation. Professional cleanings at regular intervals allow your dental team to remove calculus that forms around the implant base. During these visits, they also check the integrity of the implant crown, the health of the surrounding bone on X-ray, and any early signs of tissue inflammation that you might not notice at home.
Source: Omni Dental & Medspa
The American Academy of Implant Dentistry recommends that implant patients return for professional maintenance every three to six months, especially in the first two years after placement. This schedule can be adjusted based on how your tissue responds over time.
Signs Your Current Routine Isn’t Working
Sometimes patients feel their implant is fine because there’s no visible problem. But peri-implantitis often progresses silently in its early stages. Pay attention to:
- Bleeding or swelling around the implant, especially when cleaning
- Gum tissue that looks pulled back or lower than it used to be
- A feeling of looseness, even mild
- Persistent bad breath that doesn’t improve with brushing
These aren’t signs to wait on. Early intervention is far more straightforward than treating advanced bone loss around an implant.
Dental implants have a reported long-term success rate of over 95% when properly cared for. That statistic isn’t automatic — it’s the result of good placement combined with consistent, appropriate maintenance. The procedure gives you the foundation. Your hygiene plan is what protects it.
If you’ve been managing with general dental advice rather than a care plan specifically built around your implants, it’s worth revisiting. A conversation with your care team about what your routine should actually look like could be the most practical step you take for your long-term oral health.
Reach out to schedule a hygiene consultation and make sure your care plan is working as hard as your implants are.
People Also Ask
Your hygiene routine actually begins the day of your procedure. Your care team will give you immediate post-op instructions, but a full, long-term personalized plan is typically established at your first follow-up visit once initial healing has begun — usually within the first two weeks.
Yes, most electric toothbrushes are safe for implants, but look for one with a pressure sensor. Aggressive brushing around implant crowns can irritate the surrounding gum tissue over time. Your hygiene plan should specify the right setting and technique for your implant type.
Left untreated, peri-implantitis can lead to progressive bone loss around the implant. In advanced cases, the implant may need to be removed. This is why regular professional check-ups, not just home care, are a non-negotiable part of implant maintenance.
Yes. With a bridge, cleaning underneath the prosthetic requires specialized tools such as floss threaders or interproximal brushes to reach the area between the gums and the underside of the bridge. This area is easy to neglect with regular flossing alone, which is why it’s specifically addressed in a personalized plan.
Smoking significantly impairs blood flow to the gum tissue, slowing healing, reducing the effectiveness of your immune response to bacteria, and increasing the likelihood of peri-implantitis. Studies have shown that smokers have implant failure rates two to three times higher than non-smokers. If you smoke, this should be a frank part of your hygiene conversation with your care team.